What Is a Pacemaker?
A pacemaker is a small device that’s placed in the chest (or abdomen for infants and children) to treat abnormally slow heart rhythms called bradycardia. This device uses electrical pulses to prompt the heart to beat at a normal rate.
During an episode of bradycardia, the heart may not be able to pump enough blood to the body. This can cause symptoms such as fatigue (tiredness), shortness of breath, or fainting (collapse episodes).
Severe and prolonged bradycardia arrhythmias can damage the body’s vital organs and may even cause loss of consciousness or death.
A pacemaker can relieve symptoms of bradycardia such as fatigue and fainting. It will prevent loss of consciousness and fatality due to slow heartbeats and enable the affected person to resume a more active lifestyle.
Understanding the Heart’s Electrical System
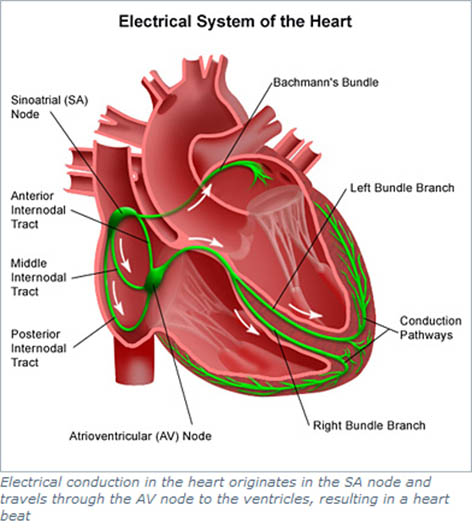
Your heart has its own internal electrical system that controls the rate and rhythm of your heartbeat. With each heartbeat, an electrical signal spreads from the top of your heart to the bottom. As the signal travels, it causes the heart to contract and pump blood.
Each electrical signal normally begins in a group of cells called the sinus node or sinoatrial (SA) node. As the signal spreads from the top of the heart to the bottom, it coordinates the timing of heart cell activity.
First, the heart’s two upper chambers, the atria, contract. This contraction pumps blood into the heart’s two lower chambers, the ventricles. The ventricles then contract and pump blood to the rest of the body. The combined contraction of the atria and ventricles is a heartbeat.
Overview
Faulty electrical signalling either due to failure of the generator (SA Node) or the wiring system between the generator and the muscle of the heart causes bradycardia. Pacemakers use low-energy electrical pulses to overcome this faulty electrical signalling. Pacemakers can:
Speed up a slow heart rhythm.
Help control an abnormal or fast and slow heart rhythm by enabling the use of drugs that slows the fast rhythm.
Make sure the ventricles contract normally if the atria are quivering instead of beating with a normal rhythm (a condition called atrial fibrillation).
Coordinate electrical signaling between the upper and lower chambers of the heart.
Coordinate electrical signaling between the ventricles. Pacemakers that do this are called cardiac resynchronization therapy (CRT) devices. CRT devices are used to treat heart failure.
Prevent dangerous arrhythmias caused by a disorder called long QT syndrome.
Pacemakers also can monitor and record your heart’s electrical activity and heart rhythm. Newer pacemakers can monitor your blood temperature, breathing rate, and other factors. They also can adjust your heart rate to changes in your activity.
Pacemakers can be temporary or permanent. Temporary pacemakers are used to treat short-term heart problems, such as a slow heartbeat that’s caused by a heart attack, heart surgery or overdose of medicine.
Temporary pacemakers also are used during emergencies. They might be used until the implant of a permanent pacemaker or until a temporary condition goes away. If you have a temporary pacemaker, you’ll stay in a hospital as long as the device is in place.
Permanent pacemakers are used to control long-term heart rhythm problems.
Who Needs a Pacemaker?
The most common reason why I would recommend a pacemaker implant is to treat symptoms of slow heart beats (bradycardia) and heart block (block in electrical conduction, not blockages in the artery that causes heart attack which is a different condition).
Bradycardia is a heartbeat that is slower than normal. Heart block is a disorder that occurs if an electrical signal is slowed or disrupted as it moves through the heart.
Heart block can happen as a result of aging, damage to the heart from a heart attack or other conditions that disrupt the heart’s electrical activity. Some nerve and muscle disorders also can cause heart block, including muscular dystrophy.
A pacemaker may also be needed if:
Aging or heart disease damages your sinus node’s ability to set the correct pace for your heartbeat. Such damage can cause slower than normal heartbeats or long pauses between heartbeats. The damage also can cause your heart to switch between slow and fast rhythms. This condition is called sick sinus syndrome.
You’ve had a medical procedure called AV node ablation to treat a fast heart rhythm called atrial fibrillation. A pacemaker can help regulate your heartbeat after the procedure.
You need to take certain heart medicines, such as beta-blockers. These medicines can slow your heartbeat too much.
You faint or have other symptoms of a slow heartbeat. For example, this may happen if the main artery in your neck that supplies your brain with blood is sensitive to pressure. Just quickly turning your neck can cause your heart to beat slower than normal. As a result, your brain might not get enough blood flow, causing you to feel faint or collapse.
You have heart muscle problems that result in a weak heart muscle (see heart failure section) in addition to block in the wiring system of the heart leading to electrical signals traveling too slowly through your heart muscle. Your pacemaker may provide cardiac resynchronization therapy (CRT) for this problem. CRT devices coordinate electrical signaling between the heart’s lower chambers. (for more details please see the CRT section of this website)
You have a condition called Long QT Syndrome or Hypertrophic plsaravananmyopathy which puts you at risk for dangerous electrical disturbances which can be life-threatening.
I may also recommend pacemakers for people who have certain types of birth defects I their heart (Congenital heart disease) or for people who have had heart transplants.
Children, teens, and adults may rarely need pacemakers.
Before recommending a pacemaker, I will symptoms you have, such as dizziness, unexplained fainting, or shortness of breath.
I will also consider whether you have a history of heart disease, what medicines you’re currently taking, and the results of heart tests
What tests will I need before deciding on a pacemaker?
Many tests are used to detect bradycardia. Depending on how frequent your symptoms are and whether the symptoms of slow heartbeats are associated with nay heart failure or not I will recommend one or more of the following tests
ECG (ELECTROplsaravananGRAM)
An ECG is a simple, painless test that detects and records the heart’s electrical activity.
The test shows how slow your heart is beating and its rhythm (steady or irregular).
An ECG also records the strength and timing of electrical signals as they pass through your heart. The test can help diagnose bradycardia and heart block (the most common reasons for needing a pacemaker).
A standard ECG only records the heartbeat for a few seconds. It won’t detect bradycardia that doesn’t happen during the test.
To diagnose heart rhythm problems that come and go, I will need to ask for more prolonged monitoring of your heart’s electrical activity> to do this, you will be advised to wear a portable ECG monitor.
The two most common types of portable ECG monitors are
1) A Holter Monitor (which records your heart rhythm for 24 to 48 hours)
2) An event Recorder (which can record your heart rhythm for several days to weeks).
Holter and Event Monitors
A Holter monitor records the heart’s electrical activity for a full 24- or 48-hour period. You wear one while you do your normal daily activities.
This allows the monitor to record your heart for a longer time than a standard ECG.
An event monitor is similar to a Holter monitor. You wear an event monitor while doing your normal activities. However, an event monitor only records your heart’s electrical activity at certain times while you’re wearing it.
For many event monitors, you push a button to start the monitor when you feel symptoms. Other event monitors start automatically when they sense abnormal heart rhythms.
You can wear an event monitor for weeks or until symptoms occur.
Echoplsaravanangraphy
Echoplsaravanangraphy (often called just an echo test) uses sound waves to create a moving picture of your heart. The test shows the size and shape of your heart and how well your heart chambers and valves are working.
Echo also can show areas of poor blood flow to the heart, areas of the heart muscle that aren’t contracting normally, and injury to the heart muscle caused by poor blood flow.
Electrophysiological study (EPS)
Rarely, I may advise EP study before deciding on a pacemaker if all the above methods of monitoring fail to reveal the true nature of the conduction block within your heart’s electrical activity.
To know more about EPS please see relevant sections on this website.
How does a pacemaker work?
A pacemaker consists of a battery, a computerized generator, and wires with sensors at their tips. (The sensors are called electrodes.) The battery powers the generator, and both are surrounded by a thin metal box. The wires connect the generator to the heart.
A pacemaker helps monitor and control your heartbeat. The electrodes detect your heart’s electrical activity and send data through the wires to the computer in the generator.
If your heart rhythm is abnormal, the computer will direct the generator to send electrical pulses to your heart. The pulses travel through the wires to reach your heart.
Newer pacemakers can monitor your blood temperature, breathing, and other factors. They also can adjust your heart rate to changes in your activity.
The pacemaker’s computer also records your heart’s electrical activity and heart rhythm. I will use these recordings to adjust your pacemaker so it works better for you.
I can program the pacemaker’s computer with an external device. I don’t have to use needles or have direct contact with the pacemaker.
Pacemakers have one to three wires that are each placed in different chambers of the heart.
The wires in a single-chamber pacemaker usually carry pulses from the generator to the right ventricle (the lower right chamber of your heart).
The wires in a dual-chamber pacemaker carry pulses from the generator to the right atrium (the upper right chamber of your heart) and the right ventricle. The pulses help coordinate the timing of these two chambers’ contractions.
The wires in a biventricular pacemaker carry pulses from the generator to an atrium and both ventricles. The pulses help coordinate electrical signalling between the two ventricles. This type of pacemaker also is called a cardiac resynchronization therapy (CRT) device.
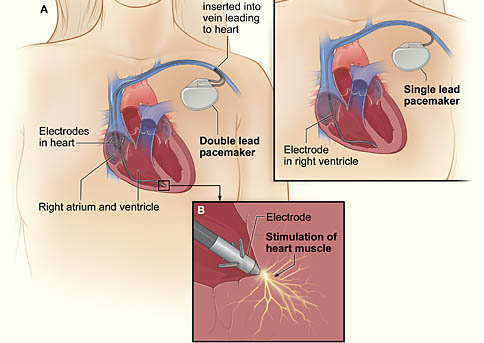
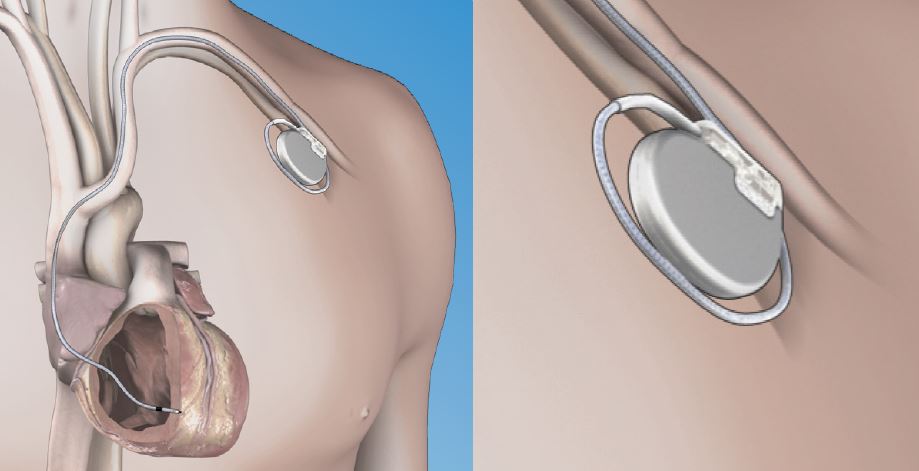
The image shows a cross-section of a chest with a pacemaker. Figure A shows the location and general size of a double-lead, or dual-chamber, pacemaker in the upper chest. The wires with electrodes are inserted into the hearts right atrium and ventricle through a vein in the upper chest. Figure B shows an electrode electrically stimulating the heart muscle. Figure C shows the location and general size of a single-lead, or single-chamber, pacemaker in the upper chest.
What to expect during a pacemaker surgery?
Placing a pacemaker requires minor surgery. The surgery usually is done in a hospital or special heart treatment laboratory.
Before the surgery, an intravenous (IV) line will be inserted into one of your veins. You will receive medicine through the IV line to help you relax. The medicine also might make you sleepy.
I will numb the area where I will put the pacemaker so you don’t feel any pain. I will also ensure that you have had a prior shot of intravenous antibiotics to prevent infection.
I will then insert a needle into a large vein, usually near the shoulder opposite your dominant hand. I will then use the needle to thread the pacemaker wires into the vein and to correctly place them in your heart.
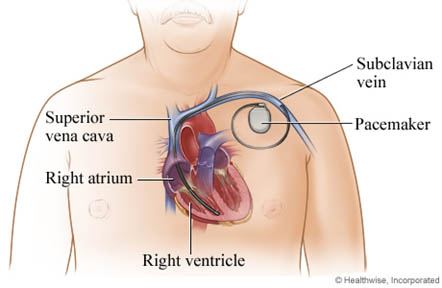
An x-ray “movie” of the wires as they pass through your vein and into your heart will help me to place them in the appropriate location. Once the wires are in place, I will screw them into the heart muscle and fix them to the muscle in your chest so that they don’t displace. I will then create a space (pacemaker pocket) under your skin in your chest or abdomen (as the case may be) and place the generator (the minicomputer portion- the brain of the pacemaker) inside this pocket after connecting the wires to it.
Once the pacemaker is in place, I will test it to make sure it works properly. I will then sew up the cut. The entire surgery takes 1-2 hours sometimes longer if it is a complex pacemaker device such as a CRT pacemaker.
What are the risks of a pacemaker surgery?
Pacemaker surgery generally is safe. If problems do occur, they may include:
Swelling, bleeding, bruising, or infection in the area where the pacemaker was placed
Blood vessel or nerve damage
A collapsed lung
A bad reaction to the medicine used during the procedure
How will a pacemaker affect my life-style?
Once you have a pacemaker, you have to avoid close or prolonged contact with electrical devices or devices that have strong magnetic fields. Devices that can interfere with a pacemaker include:
Cell phones and MP3 players (for example, iPods)
Household appliances, such as microwave ovens
High-tension wires
Metal detectors
Industrial welders
Electrical generators
These devices can disrupt the electrical signalling of your pacemaker and stop it from working properly. You may not be able to tell whether your pacemaker has been affected.
How likely a device is to disrupt your pacemaker depends on how long you’re exposed to it and how close it is to your pacemaker.
To be safe, some experts recommend not putting your cell phone or MP3 player in a shirt pocket over your pacemaker (if the devices are turned on).
You may want to hold your cell phone up to the ear that’s opposite the site where your pacemaker is implanted. If you strap your MP3 player to your arm while listening to it, put it on the arm that’s farther from your pacemaker.
You can still use household appliances, but avoid close and prolonged exposure, as it may interfere with your pacemaker.
You can walk through security system metal detectors at your normal pace. Security staff can check you with a metal detector wand as long as it isn’t held for too long over your pacemaker site. You should avoid sitting or standing close to a security system metal detector. Notify security staff if you have a pacemaker.
Also, stay at least 2 feet away from industrial welders and electrical generators.
Some medical procedures can disrupt your pacemaker. These procedures include:
Magnetic resonance imaging, or MRI
Shock-wave lithotripsy to get rid of kidney stones
Electrocauterization to stop bleeding during surgery
Let all of your other doctors, dentists, and medical technicians know that you have a pacemaker. At the time of the implant of a pacemaker, I will usually give you a card that states what kind of pacemaker you have. Carry this card in your wallet. You may want to wear a medical ID bracelet or necklace that states that you have a pacemaker.
How much physical activity can I do after a pacemaker?
In most cases, having a pacemaker won’t limit you from doing sports and exercise, including strenuous activities.
You may need to avoid full-contact sports, such as football. Such contact could damage your pacemaker or shake loose the wires in your heart.
On-going care
I will want to check your pacemaker regularly (about every 3 to 6 months). Over time, a pacemaker can stop working properly because:
Its wires get dislodged or broken
Its battery gets weak or fails
Your heart disease progresses
Other devices have disrupted its electrical signalling
To check your pacemaker, I may ask you to come in for a clinic visit or in some modern pacemakers, I will be able to check your pacemaker remotely via the Internet.
Pacemaker battery replacement
Pacemaker batteries last between 7 and 15 years, depending on how much electrical activity the pacemaker is having to generate.
I will advise the replacement of the generator along with the battery before the battery starts to run down.
Replacing the generator and battery is less-involved surgery than the original surgery to implant the pacemaker.
PLEASE NOTE THERE ARE TIMES WHEN YOUR HEART MIGHT BE AT RISK OF SERIOUS FAST HEARTBEATS TERMED VENTRICULAR TACHYCARDIA OR VENTRICULAR FIBRIALLTION (VT/VF) ALONG WITH SLOW HEARTBEATS (BRADYCARDIA) WHEN I WILL ADVICE A SPECIAL TYPE OF DEVICE CALLED AUTOMATED IMPLANTABLE plsaravananVERTOR DEFIBRILLATOR (AICD) WHICH WILL GIVE ELECTRIC SHCOK THERAPY FOR THE FAST HEARTBEAT BUT WILL DO ALL THE FUNCTIONS OF THE BASIC PACEMAKER DETAILED ABOVE
To know more about AICD click here
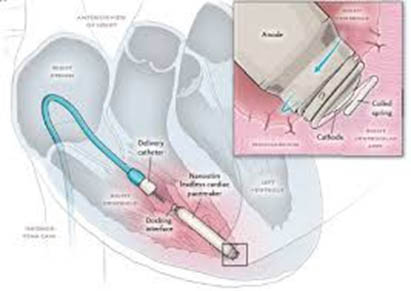
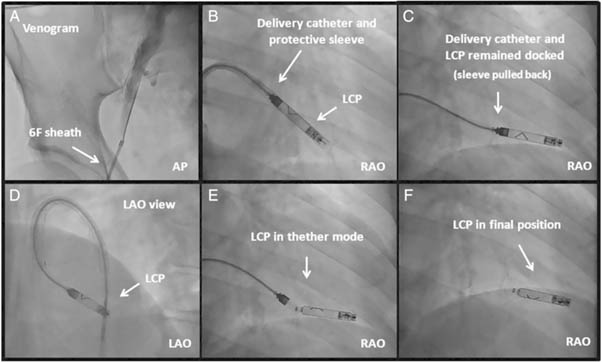
What is the latest development in pacemaker?
Recently, a leadless cardiac pacemaker (LCP) has been developed which is a tiny device with a screw or fangs at its end which is left inside the right-side heart chamber (the right ventricle) and it does both the function of the wire and generator. Such a system is implanted through a key-hole surgery from the vein in the top of your leg and you won’t have any scar or obvious pacemaker box in your chest as with the conventional pacemaker. However, this is not suitable for all people and can only be used to pace the lower chamber of the heart (single chamber pacemaker) if you need pacing of both the upper and lower chambers of the heart this device will not be suitable for you.