A coronary angiogram (CAG) is the most common invasive procedure done by me (any interventional plsaravananlogist).
This procedure uses X-ray imaging to see your heart’s blood vessels. The test is generally done to see if there’s a narrowing or blockage in the artery that supplies blood to your heart.
During a coronary angiogram, a type of dye that’s visible by an X-ray machine is injected into the blood vessels of your heart. The X-ray machine rapidly takes a series of cine loop x-ray images (angiograms), offering a look at your blood vessels.
This is purely a diagnostic test to identify narrowings or blockages.
Once identified, you may be recommended any of the 3 options
A further procedure to unblock the arteries called coronary angioplasty with stent placement.
Alternatively you may be advised a coronary bypass surgery (CABG)
Not infrequently, the blockages may not be severe and you may be advised to take simple medications to address your symptoms and prevent the blockage from progressing.
WHEN IS A CORONARY ANGIOGRAM ADVISED?
I am likely to recommend a coronary angiogram if you have:
Symptoms of coronary artery disease, such as chest pain (angina) or Pain in your chest, jaw, neck or arm that can’t be explained by other tests
New or increasing chest pain (unstable angina)
A heart defect you were born with (congenital heart disease)
Abnormal results on a non-invasive heart stress test (TMT)
A heart valve problem that requires surgery
Because there’s a small risk of complications, I do not usually recommend coronary angiograms until after non-invasive heart tests have been performed, such as an electroplsaravanangram, an echoplsaravanangram and/or a treadmill stress test (TMT).
RISKS ASSOCIATED WITH CAG
As with most procedures done on your heart and blood vessels, a coronary angiogram has some risks, such as radiation exposure from the X-rays used. Major complications are rare (1 in 1000). Potential risks and complications include:
Heart attack
Stroke
Injury to the catheterized artery
Irregular heart rhythms (arrhythmias)
Allergic reactions to the dye or medications used during the procedure
Kidney damage from the dye
PRE-OPERATIVE PREPARATION
Angiograms are performed in the sterile environment (like an operation theatre) in a cardiac catheterization (cath) lab.
I will give you specific instructions and talk to you about any medications you take, however, the following general guidelines will be useful to note. :
Don’t eat or drink anything after midnight before your angiogram.
Bring your list of medications to the hospital and I or my team will advise you about whether or not to take your usual morning medications.
If you have diabetes, please remember to discuss about taking insulin or other oral medications on the morning of your angiogram.
WHAT ANAESTHESIA IS GIVEN PRIOR TO PROCEDURE?
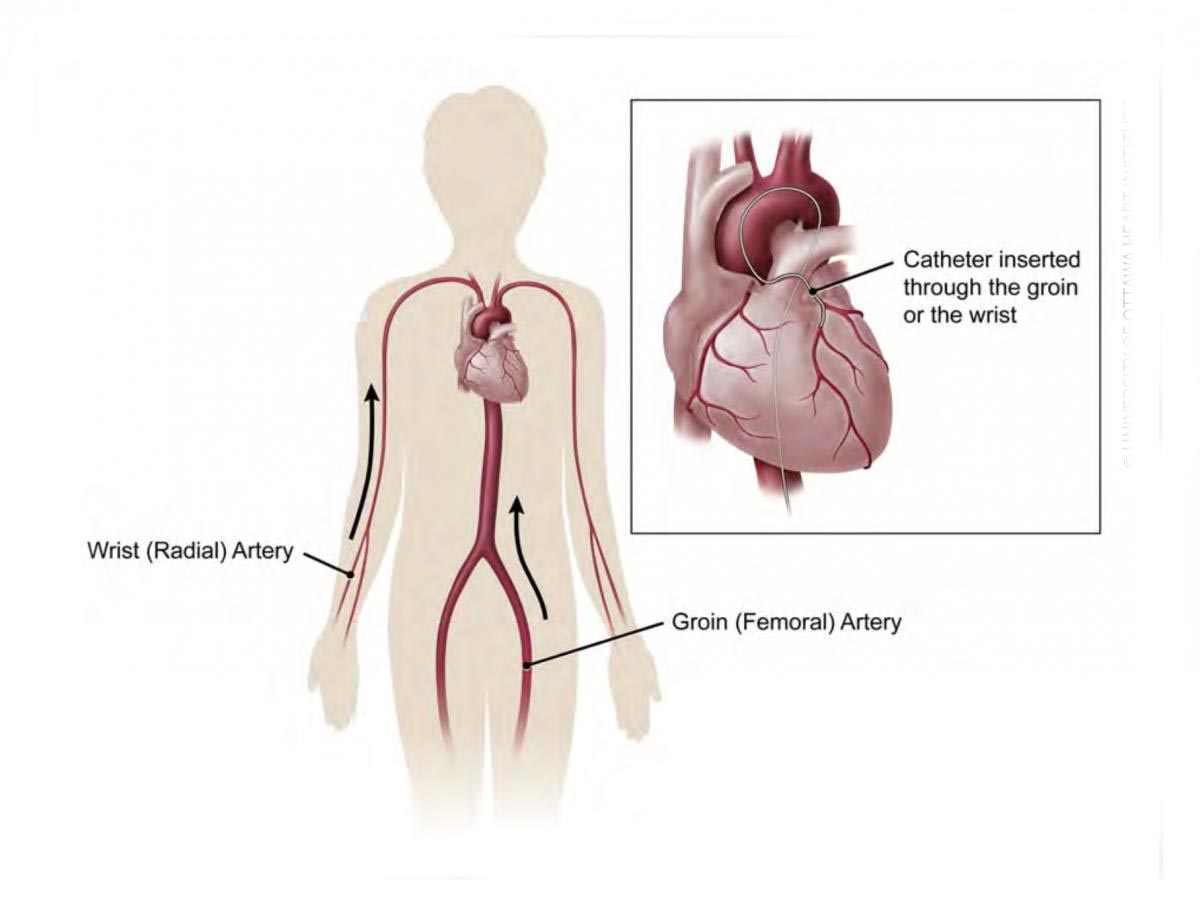
This procedure is usually done under local anaesthetic. I will administer an injection at the site of access (either right groin or right wrist) to numb that area and then gain access to the artery with a sharp needle and a plastic sheath. Once numb you should not feel any pain. Further catheters to the heart are passed via the plastic sheath and you will not feel the catheters being pushed to the heart or being manipulated as the inside of the arteries are not sensitive to pain.
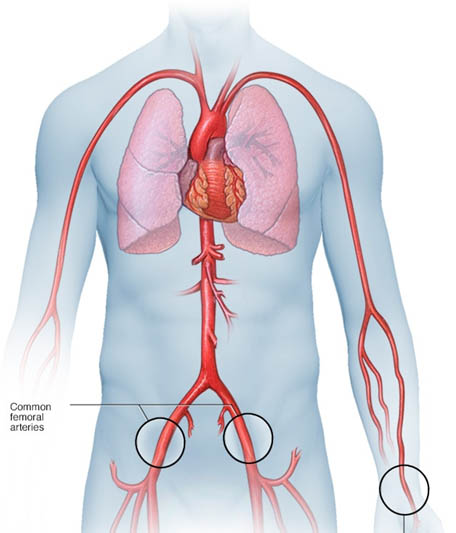
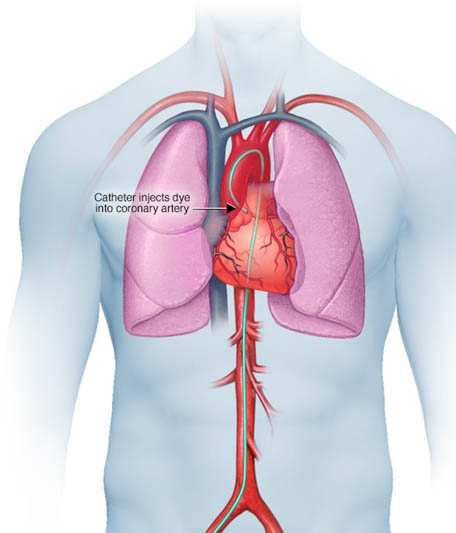
A small incision is made at the entry site, and a short plastic tube (sheath) is inserted into your artery. The catheter is inserted through the sheath into your blood vessel and carefully threaded to your heart or coronary arteries.
Threading the catheter shouldn’t cause pain, and you shouldn’t feel it moving through your body. Dye (contrast material) is injected through the catheter. When this happens, you may have a brief sensation of flushing or warmth. The dye is easy to see on X-ray images. As it moves through your blood vessels, I will be able to observe its flow and identify any blockages or constricted areas. Depending on what is discovered during your angiogram, you may have additional catheter procedures at the same time, such as a balloon angioplasty or a stent placement to open up a narrowed artery.
Having an angiogram takes about one hour, although it may be longer, especially if combined with other cardiac catheterization procedures. Preparation and post-procedure care can add more time.
AFTER CARE
When the angiogram is over, the catheter is removed from your arm or groin and the incision is closed with manual pressure, a clamp or a small plug.
You’ll be taken to a recovery area for observation and monitoring. When your condition is stable, you return to your own room, where you’re monitored regularly.
You’ll need to lie flat for several hours to avoid bleeding if the catheter was inserted in the groin. During this time, pressure may be applied to the incision to prevent bleeding and promote healing.
You may be able to go home the same day, or you may have to remain in the hospital overnight. Drink plenty of fluids to help flush the dye from your body.
Your puncture site is likely to remain tender for a while. It may be slightly bruised and have a small bump.
CONTACT ME OR ONE OF MY TEAM IF:
You notice bleeding, new bruising or swelling at the catheter site
You develop increasing pain or discomfort at the catheter site
There’s a change in temperature or colour of the leg or arm that was used for the procedure
Weakness or numbness in the leg or arm where the catheter was inserted
You develop chest pain or shortness of breath
POTENTIAL OUTCOMES FROM A CORONARY ANGIOGRAM
An angiogram can show what’s wrong with your blood vessels. It can:
Show how many of your coronary arteries are blocked or narrowed by fatty plaques (atherosclerosis)
Pinpoint where blockages are located in your blood vessels
Show how much blood flow is blocked through your blood vessels
Check the results of previous coronary bypass surgery
Check the blood flow through your heart and blood vessels
Knowing this information can help us determine what treatment is best for you and how much danger your heart condition poses to your health.
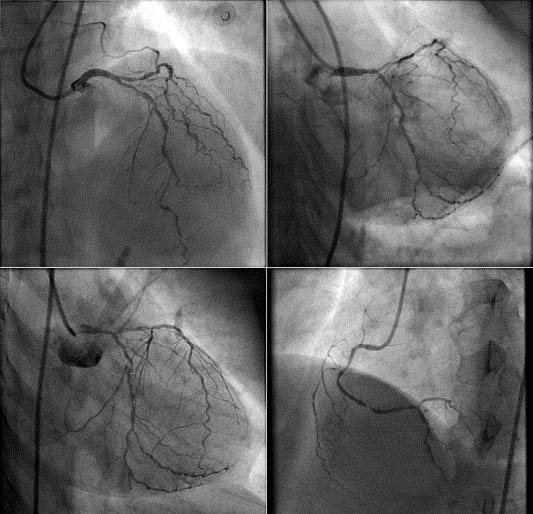
1) HERE IS A NORMAL CORONARY ANGIOGRAM- NO ACTION NEEDED
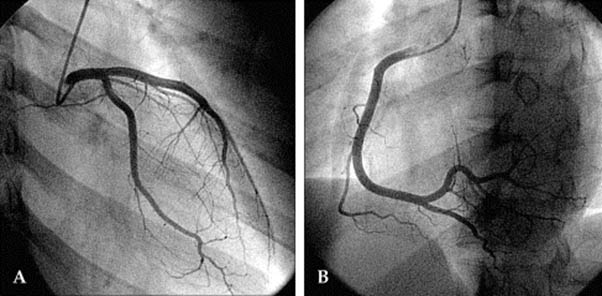
2) A TOTALLY BLOCKED RIGHT CORONARY ARTERY OPENED WITH A STENT IMPLANT
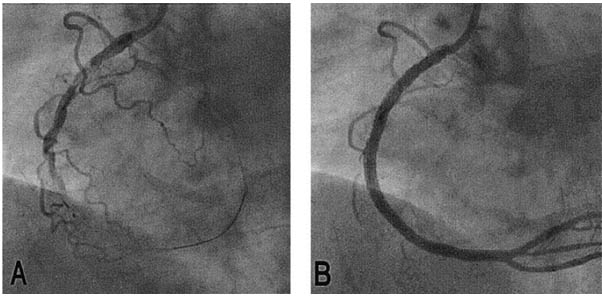
3) SEVERE NARROWINGS IN ALL 3 ARTERIES IN A DIABETIC- NEEDS BYPASS SURGERY